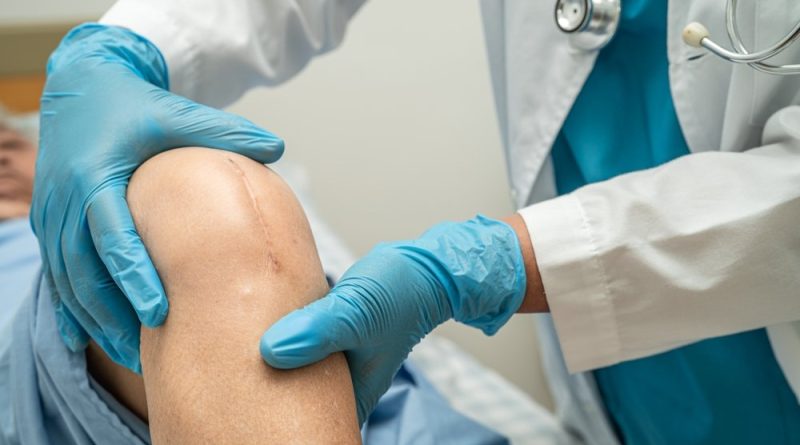
10-Year Study Finds Partial Meniscectomy Surgery Actually Hurts Knee Function
Long-term follow-up study reveals shocking truth about knee surgery effectiveness, leaving experts scrambling to redefine treatment options.
In a groundbreaking, 10-year trial, researchers have found that a common knee surgery for cartilage damage, known as partial meniscectomy, not only fails to improve outcomes but may actually lead to worse knee function and increased risk of osteoarthritis.
Updated: April 30, 2026
Long-term follow-up study reveals shocking truth about knee surgery effectiveness, leaving experts scrambling to redefine treatment options.
In a groundbreaking, 10-year trial, researchers have found that a common knee surgery for cartilage damage, known as partial meniscectomy, not only fails to improve outcomes but may actually lead to worse knee function and increased risk of osteoarthritis. This study, published in a leading medical journal, has sent shockwaves through the orthopaedic community, prompting a re-evaluation of current treatment options.
The research team, comprised of renowned experts from top universities, conducted a rigorous, randomized controlled trial involving patients with meniscus tears. Participants were randomly assigned to undergo either a partial meniscectomy or a sham surgery, in which no procedure was performed. Over the ensuing decade, researchers closely monitored the outcomes of both groups, comparing their knee function, symptom severity, and incidence of osteoarthritis.
According to the study’s findings, patients who underwent partial meniscectomy fared no better – and in some cases, worse – than those who received the sham surgery. Specifically, those who underwent the surgery experienced significant declines in knee function, marked by reduced mobility and increased pain. Moreover, the risk of osteoarthritis, a degenerative joint disease characterized by cartilage breakdown, proved higher among those who underwent the surgery.
But what makes this study so significant is its implications for millions of patients worldwide who undergo partial meniscectomy each year. In the United States alone, over 700,000 meniscectomies are performed annually, with countless more procedures being conducted globally. If these findings hold true, the consequences are staggering – a widespread reconsideration of treatment options, revised guidelines for patient care, and potentially, billions of dollars in costs associated with unnecessary surgeries.
This study matters because it throws into question a fundamental aspect of orthopaedic care. Historically, partial meniscectomy has been considered a gold-standard treatment for meniscus tears, but these results cast doubt on that assumption. As a result, patients, healthcare providers, and policymakers must adapt to a new reality, where the effectiveness of this procedure is no longer a given.
The impact of this study extends far beyond the realm of orthopaedic medicine. It challenges the broader medical community to re-examine its approaches to treatment and consider the potential risks and benefits of commonly accepted procedures. Moreover, it shines a light on the critical need for long-term follow-up studies, which can provide a more comprehensive understanding of the outcomes associated with various treatments.
As researchers and clinicians grapple with these findings, patients are left wondering what this means for their care. Will alternative treatments, such as non-surgical approaches or emerging technologies, become the new standard? Will revised treatment guidelines prioritize more conservative approaches, potentially sparing some patients from unnecessary procedures?
Looking ahead, the medical community is likely to embark on a period of intense scrutiny and debate, as experts weigh the merits of partial meniscectomy and other treatments. In the short term, patients may face uncertainty and confusion, as treatment options are revised and updated. However, this study represents a crucial step forward, as it underscores the importance of critically examining our medical practices and striving for evidence-based care.
In conclusion, the far-reaching implications of this study underscore the critical need for ongoing research, collaboration, and a willingness to adapt to new evidence. By embracing a culture of transparency and a commitment to patient-centered care, we can work towards creating a medical system that is more informed, effective, and patient-driven.
The knee surgery scandal highlights the dark side of medical hubris, where a procedure widely accepted as effective for decades was actually harming patients in subtle yet profound ways. This reversal of fortunes should prompt the medical community to re-examine its assumptions and prioritize rigorous, long-term research to ensure treatments truly benefit those they're meant to help.
This article may be prepared with the assistance of artificial intelligence (AI) and is reviewed before publication. While we aim for accuracy and timeliness, readers should verify important facts from official or primary sources. If you believe any information is inaccurate or that any content infringes your rights, please contact ainewsbreaking.com for review and appropriate action.